Porphyrias are a group of disorders caused by a malfunctioning enzyme of the heme biosynthetic pathway. Depending on the altered enzyme, there are several types of disorder, each with different Porphyria symptoms.
Introduction
Porphyrias are a rare group of disorders caused by an alteration in one of the enzymes responsible for the biosynthesis of heme, which is a molecule mostly found in blood, in the liver and in bone marrow. When one of the enzymes responsible for heme production is not properly functioning, the heme precursors, porphyrins, accumulate in some areas of the body, causing disorders that can range from cutaneous disorders to neurological disorders.
Heme Production
There are eight enzymes that play a role in the biosynthetic pathway leading to heme production, with four being located in the mitochondria and four in the cytosol. Any kind of alteration in any of these enzymes can cause the insurgence of one of the types of Porphyria. The information necessary to make each of these enzymes is encoded by a specific gene. Specifically, the genes that are responsible for each enzyme of the heme biosynthetic pathway and, consequently, for any malfunctioning of such enzymes are the ALAD, ALAS2, CPOX, FECH, HFE, HMBS, PPOX, UROD and UROS genes.
Types of Porphyrias
The most common classification of Porphyrias is based on the region of the body where there is an excessive production and accumulation of porphyrins and on the types of symptoms that are caused; based on this classification, Porphyrias are divided into acute (or hepatic) porphyrias and cutaneous porphyrias.
Acute porphyrias occur mostly when porphyrins accumulate in the liver. Patients affected by acute porphyria experience muscle pain, pain in the abdominal area and vomiting. This type of porphyria also has several other implications at a neurological level, however, as patients may suffer from hallucinations, paranoia, depression and anxiety. These types of porphyrias are also called acute because the episodes during which the signs and symptoms occur appear quickly and do not usually last long. Types of acute porphyrias are acute intermittent porphyria and erythropoietic porphyria.
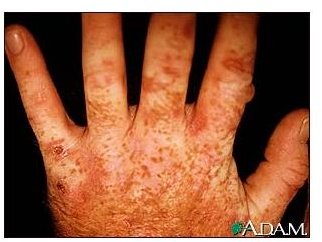
Cutaneous porphyrias, instead, mainly target the skin, making it more sensitive to exposure to light (increased photosensitivity). Those affected by cutaneous porphyrias suffer from blisters, erythema, and even necrosis of the skin when they are exposed to sunlight. This type of porphyria has been one of the main sources of inspiration for the legends of vampires, who are described as supposedly non-human creatures that are deathly “allergic” to sunlight. Some types of porphyrias belonging to this category are porphyria cutanea tarda and hepatoerythropioetic porphyria.
Even rarer are neurocutaneous porphyrias, which are conditions that affect both the skin and the nervous system , where neurological episodes are triggered by exposure to sunlight. Types of neurocutaneous porphyrias are variegate porphyria and hereditary coproporphyria.
How is Porphyria Inherited?
Inheritance seems to play some kind of role in the development of porphyrias. So how is Porphyria inherited? The pattern of inheritance can include both autosomal dominant inheritance , where the defective gene is only inherited from one parent, and autosomal recessive inheritance, where the defective gene is inherited from both parents. However, it has been noticed that only one person in every ten who has the faulty gene actually develops the disease. This means that there are environmental factors which trigger the disease in those individuals who are genetically predisposed to it.
There are various external factors that may be responsible for the onset of porphyrias, and while their nature may seem quite different, they have in common the fact that they all cause an increase in heme production. The most common external factors that can lead to porphyrias are sedatives, contraceptives, tranquillizers, barbiturates, alcohol consumption, certain types of hormones, smoking, hepatitis C and even HIV infection.
Diagnosis and Treatment
Once porphyria symptoms are detected, a diagnosis is made by performing tests on blood, urine and stool to monitor the level of porphyrins. It is important that these analyses are performed when an acute attack is in progress; otherwise there is a very high risk of obtaining false results.
Patients who suffer from acute porphyrias are usually treated with pain medications and with hematin, which is another type of heme that can be used by the body. Moreover, a diet rich in carbohydrates and, during acute attacks, a 10% glucose infusion are also used as a treatment for Porphyrias. Patients suffering from cutaneous porphyrias are usually treated with administrations of activated charcoal, which helps in absorbing excess porphyrins. Some individuals may also require blood removal, a process called phlebotomy, in order to lower the amount of iron, which will lead to a decrease in the amount of porphyrins.
Since, as of now, there is no outright cure for the porphyrias, patients are taught how to learn to live with whichever of the types they may have. Most importantly, they are taught about avoid any known triggers, such as alcohol and smoking. They are also advised to take precautions to protect their skin with long-sleeved tops and long pants, as well as scarves and sunscreen to cover other parts of their body.