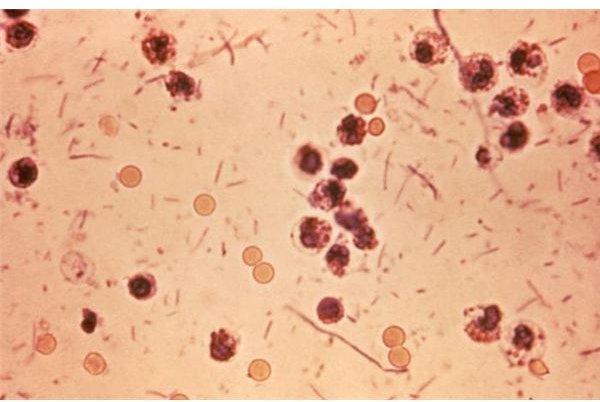
Shigella is a Gram-negative non-spore forming rod-shaped bacteria. It is a close relation of E. coli and Salmonella and can infect the gut to cause a number of gastrointestinal problems.
Shigella Bacteria
A shigella infection can start with the ingestion of only a few bacterial organisms ; that number can even be as low as 10 depending on the age and general health of the individual. Shigella bacteria cause Shigellosis, also known as bacillary dysentery.
Symptoms of a shigella infection can include: -
- Abdominal cramps
- Diarrhoea - with blood and mucus in the stools
- Dehydration
- Fever
- Rectal pain
The diarrhoea can range in severity from mild to severe. And in some instances it may be so painful that a person will require hospital treatment.
Up to 3% of individuals infected by Shigella will develop Reiter’s syndrome , which is characterised by inflammation of the eye and urethra, and joint pain. It’s also known as reactive arthritis and is caused by the immune system attacking itself instead of the pathogen.
Infectious Bacteria
Shigella bacteria are highly infectious, and spread easily amongst people via the fecal-oral route. The bacteria are present in stools and most infections occur when the germs pass from the stool to fingers of one person and then to the mouth of another. This is why basic hygiene such as hand washing is imperative to prevent the germs from spreading.
Shigella infection can also be acquired by drinking or swimming in contaminated water and by eating contaminated food. Food can become contaminated when infected people who haven’t washed their hands prepare and cook meals.
Pathogenesis
Shigella bacteria wreak their havoc by invading, multiplying and killing the cells that line the colonic mucosa. Once the bacteria are inside host cells they can trigger them to produce pro-inflammatory mediators such as interleukin 8. This helps to create a strong inflammatory response that eases the way for further bacterial invasion.
Several virulence factor genes have been indentified such as; -
icsA gene - codes for an outer membrane protein that allows the bacteria to move easily through the cytoplasm
shet2 gene - codes for an enterotoxin
Shigella bacteria adhere to host cells and more than 25 genes are involved in helping to get them across the membrane. Shigella is surrounded by a membrane-bound vacuole within the host cell which it rapidly lyses. The bacteria is then released into the cytosol where it rapidly grows and divides.
Once released the bacteria are coated in filamentous actin which forms a tail at one pole to drive the bacteria toward the plasma membrane. Once there they forms projections from the surface of the infected cell to the surface of an unaffected cell. A tip penetrates the latter and the bacteria eventually break out of the infected cell to colonise a new cell.
Some strains produce Shiga toxin and enterotoxin that have cytotoxic effects and can cause a range of problems including hemolytic uremic syndrome. This can lead to a loss of kidney function.
Treatment for Shigellosis
For most individuals the infection will clear up within a week without any complications. Shigellosis can be treated with antibiotics such as Ampicillin and cotrimoxazole. However, some pathogenic strains have developed antibiotic resistance . Fluid and salt replacement may also be necessary as the body will need to be topped up, having lost fluid and nutrients through diarrhoea.
According to the World Health Organisation (WHO) Shigellosis is endemic throughout the world with 164.7 million cases, of which 163.2 million are in developing countries. Every year approximately 1.1 million people die from the disease and 580,000 cases of Shigellosis are reported by travellers from industrialised countries. These figures were correct as of October 2009.
Once a person has been infected by Shigella they usually then become resistant to that particular strain. Although there aren’t any Shigella vaccines at the moment development is ongoing. One of the best ways of avoiding shigella infections is to adopt scrupulous hygiene regimes.
Reference
World Health Organisation - Shigella
Current Aspects of Shigella Pathogenesis