Working as a claims processor is a financially rewarding work opportunity, that doesn’t require any specialized education. A claims processor helps an insurance company with the processing of insurance claims. Read on to find out more about this type of job.
Claims Processor
If you’re looking to work from home, claims processor jobs are a great new work opportunity to explore. This job essentially entails data entry and claim analysis work, to facilitate timely reimbursement of insurance claims by the insurance companies.
A claims processor is the first point of contact for the insured customers to begin the process of financial recovery for the insured damages, from the insurance company. When working individually from home as a claims processor it is best to specialize in one or two insurance areas. All insurance companies dealing in any type of insurance – auto, life, health, house or business, require claims processor to do the ground work for prompt and accurate handling of insurance claims. Basically, the work profile of an insurance claims processor includes receiving claims, collecting the required information, feeding the data into the company’s system and even analyzing the fitness of a claim to decide whether the claim should be processed or denied. Let’s take a closer look at the job description.
Job Responsibilities
Whenever an insurance company receives a claim, either through mail or in writing, the information about the claim details are uploaded into the centralized system. This centralized system distributes the claims to all the claims processors working with the company, using a role based work distribution system. The assigning of the claims is based on:
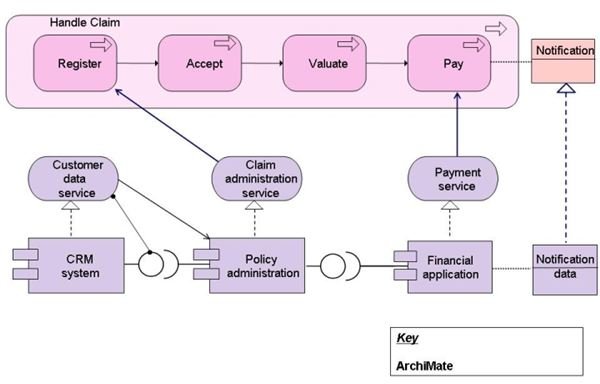
- the geographical location of the claims processor,
- the specialization of the claims processor,
- the number of claims that have been already allotted, and
- the track record of how efficiently the claims processor has handled claims in the past.
The job of the claims processor begins only when he/she is assigned a claim by the system. Here is a brief job description of what a claims processor is expected to do.
- Upon receiving the claim, it is for the claims processor to check whether the damages are covered by the insurance policy that the customer holds. This is the most vital step as no claims can be processed any further if they are not covered under the insurance policy.
- Next, the claims processor will examine the claim in terms of whether the claim was filed as per the standard accepted procedure and in a timely manner. This is the step where the claims form and all supporting documents need to be examined in details for the correctness of the information. Based on this examination the processor will assign a payment, denied or pending status to the claim request.
- If satisfied with the accuracy of the information received, the claims processor may finalize the claim. In cases, where there is need further investigation or where additional information or supporting documents may be needed for making a final decision – a pending status is awarded to the case.
Skills Required
Claims processor candidates require some basic skills.
- Customer Service Skills: Since a claims processor may have to interact directly with the insured person either on phone or through email – having good customer service and interpersonal skills is the most essential part of this job. In addition to a pleasant demeanor – this job profile calls for patience and empathy.
- Technological Skills: Since the work of a claims-processor is mostly automated, he/she should be comfortable working on a computer and using multi-line telephones.
- Data Handling Skills: A lot of typing and data entry is involved in this work, so building speed and accuracy in typing and feeding in information is very essential to succeed as a claims processor, working from home.
- Analytical Abilities: A claims processor would be able to easily investigate and analyze the claims as per the guidelines received from the company. Some basic investigative and judgment skills may be needed to determine the accuracy of the information provided in the claim.
- Problem Solving Skills: Besides handling claims, a claims processor may at times be required to handle complaints and issues related to unsettled or pending claims. Where needed, he/she may be required to resolve the problem or else pass on the case to the appropriate authorities.
Training
Claims processor jobs do not require any college degree or some specialized education, except in some states where they may be required to clear some tests before getting an insurance license. The basic educational requirement is a high school diploma, and all the required training for handling insurance claims is provided by the company on the job.
Although, adequate on the job training is provided on how to use the claims processing software and how to analyze and examine claims, those who desire to excel in this field can go in for short term courses on claims processing. These courses are all the more important if one aspires to be a medical claims processor.
Salary
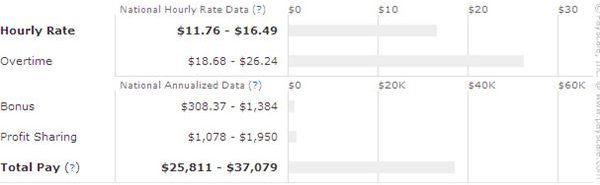
According to pay scale.com, the current national average salary for claims processors ranges between $25000 and $37000. (https://www.payscale.com/research/US/Job=Insurance _Claims_Processor/Hourly_Rate) However, these figures may vary drastically depending on the personals skills of the claims processor and the amount of time put in.
References
- Image Credit: Stubacca (http://commons.wikimedia.org/wiki/File:Home _office_small_office.JPG)
- Image Credit: Borjan & Hans Wierenga (http://commons.wikimedia.org/wiki/File:ArchiMate _sample_insurance_claim_process.jpg)
- Screenshot Taken by - Sidharth Thakur



