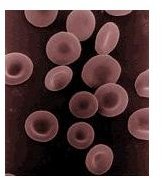
Red blood cells have a lifespan of about 120 days. In hereditary spherocytosis the lifespan of these cells is decreased due to an increased rate of RBC destruction. This article gives a short overview of the disorder and the genetic defects involved in hereditary spherocytosis.
Hereditary Spherocytosis
Hereditary spherocytosis or HS is a genetic disorder characterized by anemia, jaundice and splenomegaly. The genetic defects lie in the red cell membrane proteins causing cells to lose their surface area and become spherical in shape. They are also less flexible than normal red blood cells. When these cells pass through the spleen, they become trapped in narrow blood passages which leads to cell destruction and hemolysis (break up). Enlargement of the spleen or splenomegaly then occurs due to the build up of red blood cells.
The breakdown of RBCs leads to increase bilirubin levels in the blood causing jaundice and gallstone formation in many patients. A small percentage of HS patients may present with jaundice at birth, and require blood transfusion. About 20% to 30% of HS patients may not show signs nor symptoms of the disease, as the destruction of red blood cells can be offset by the production of new red blood cells in the bone marrow.
In most cases, however, moderate to severe hemolytic anemia becomes apparent when the compensatory mechanism is not enough.
Genetic Causes of Red Blood Cell Abnormality
HS is transmitted either as an autosomal dominant or autosomal recessive trait . It can also be caused by spontaneous mutations. The disease is most common among people from Northern Europe and those of Japanese descent.
-
Molecular defects in hereditary spherocytosis are found in the genes coding for alpha and beta spectrin (cytoskeletal proteins), band 3 protein, ankyrin and protein 4.2 leading to the formation of abnormal red blood cells. Mutations in ankyrin, beta spectrin and band 3 tend to follow an autosomal dominant pattern of inheritance, while alpha spectrin is related to recessive HS.
-
Spectrin mutation is the most common cause of HS. A point mutation is involved in alpha spectrin which leads to an amino acid substitution (alanine/aspartic acid). Another point mutation leads to a binding defect of spectrin to protein 4.1.
Advertisement -
Other genetic mutations either result in impaired synthesis of beta spectrin or the production of unstable and abnormal beta spectrin.
-
The ankyrin gene (which codes for a cell membrane protein) is located in the short arm of chromosome 8, specifically at chromosome band 8p11.2 and a deletion of the short arm or the translocation of chromosome 8 results in ankyrin defects.
Advertisement -
Mutations of protein 4.2 occurs mostly among the Japanese population leading to shape changes in red blood cells which are seen as spherocytes, elliptocytes and ovalocytes.
Symptoms of Hemolytic Anemia and Treatment
HS patients with chronic hemolytic anemia present with pallor, weakness, shortness of breath and they tire easily. There can also be jaundice, gallstone formation and spleen enlargement. Folic acid as a food supplement is given to the patient to enhance blood production. Surgical removal of the spleen may sometimes be necessary.